Success & Skepticism: Technology in the fight against COVID-19

The healthcare industry has been rattled as it continues to address the increasing demands of the pandemic. With all hands on deck, leaders in the healthcare space had to reimagine how to deliver high quality care in the craziest moment for public health in recent decades.
Along with adjustments in facilities to manage occupancy fluctuations, many healthcare systems experienced disruptions in supply chains, and the use of telehealth increased like never before as a safer alternative to in-person care. These are just a few of the challenges healthcare faced during the pandemic, many of which were mitigated by technology.
Whether in the grip of a relentless pandemic or not, industries have always turned to technology to scale initiatives, enhance the delivery of services, and compete in an evolving market. Doing so has never been more urgent than in recent months. Technology was (and remains) crucial to seeing us through these unprecedented times and has left its mark on healthcare, starting in the home.
Once limited to the confines of a doctor’s office, today the space in which healthcare is delivered is entirely different. Patients can receive care from the comfort (and safety) of their living rooms. Of course, this development isn’t unique to the pandemic, telehealth has existed for a long time, but has recently gained traction and popularity.
Leaders in the healthcare space warn of various consequences of this change. John Mendelson, MD, founder and Chief Medical Officer at Ria Health told us: “There’s no difference between the exam room in 1940 and now. The only difference is that we look at a computer. Everything else is the same. COVID-19 has allowed for the destruction of that space, as the only one to deliver an interaction.”
The challenge now is to decide what this space looks like and what kind of environment is appropriate for taking calls from home. Suppose, for instance, the person on the other end of the Zoom spots something in their patient’s living room perhaps they should not have seen. “What are the appropriate options, what is the etiquette? All this needs to be determined,” Mendelson stated. “There needs to be a protocol.”
Technology, along with transforming the space patients receive care, is enabling health care professionals and hospitals to adapt to the changing demands of the pandemic. In doing so, it has revealed gaps in the infrastructure of our healthcare system and the way we address healthcare problems. From a priorities perspective, hospitals rushing to implement new protocols identified those gaps. One solution has been to leverage artificial intelligence (AI).
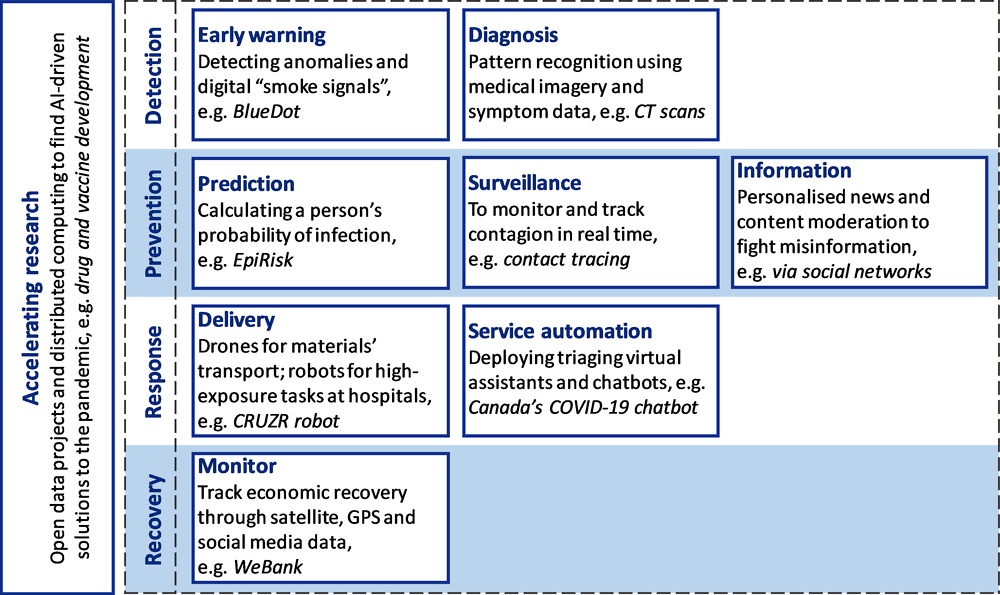
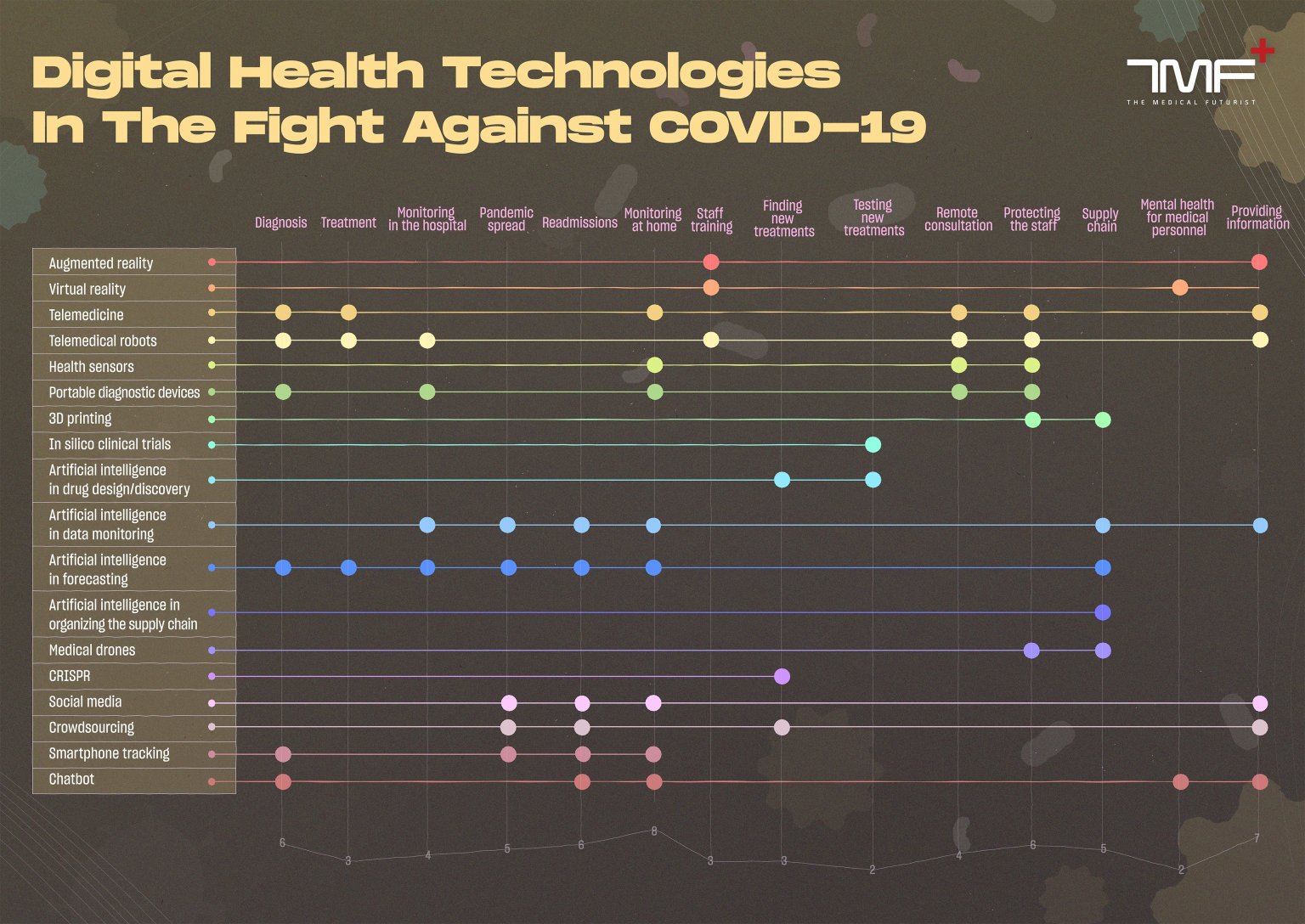
AI is not a new technology to the healthcare industry; however, COVID-19 has presented machine learning (ML) scientists the opportunity to apply their skill set to pandemic related challenges. We’ve most recently seen an uptick in AI systems developed for detection, contact tracing, hospital resource management, and drug discovery.
Detection accuracy has been very high with AI. In one case Deep Convolutional Networks were able to identify COVID-19 in CT images with 99.51% accuracy. In another case, a Convolutional Neural Network identified COVID-19 through X-ray images with 98.08% accuracy.
Various AI enabled apps have been used to perform contact tracing. These apps collect individual user data which is then analyzed by AI/ML systems to notify when a user might be at risk of exposure. Digital contact tracing is a lot faster than non-digital. 36 countries successfully deployed digital contract tracing methods, such as Australia, Austria, Finland, France, and Germany.

Despite these noteworthy developments, some remain skeptical of AI. Mendelson jokingly claims to prefer “natural stupidity,” suggesting we have yet to see an area where AI has succeeded in giving us a better solution than its human counterparts. While Mendelson sees a future for AI in image processing, as an MD he is hesitant to fully endorse it. “What can AI do that is actually transparent enough that you trust the way the answer was gotten to?” he challenged.
Another hurdle for AI is medical evidence. “The physician community is going to be weary of AI,” Mendelson said, emphasizing the need for evidence and assurance. “AI isn’t going to be accepted until there are adequately controlled studies showing it is doing something, perhaps in radiology or pathology.” Mendelson also said that AI needs to integrate physicians into the product, as there’s still a need for a “person to deliver news, be convincing, and explain what the data means.”
Then there’s the issue of noise: meaningless unnecessary data that often alters the performance of models. Noisy data is especially risky as it pertains to health. For instance, a smart watch may incorrectly indicate that the wearer has atrial fibrillation if someone other than the patient puts on the watch. This type of scenario must be accounted for.
How? We need to be able to weed out bad data. Mendelson pointed out the importance of excluding data when necessary to eliminate noise: “Excluding data is more important than including data.” This is another area where AI could be of use.
The COVID-19 pandemic forced us to reconsider some of the fundamentals of healthcare, and in doing so, explore ways technology and AI can guide the way. While there are many successes to celebrate, as always we must proceed in an informed and skeptical manner.
Take a look at our AI Healthcare Practice to learn more about how Fusemachines is bringing healthcare innovation to the next level.
For more information on Ria Health, visit their website.


